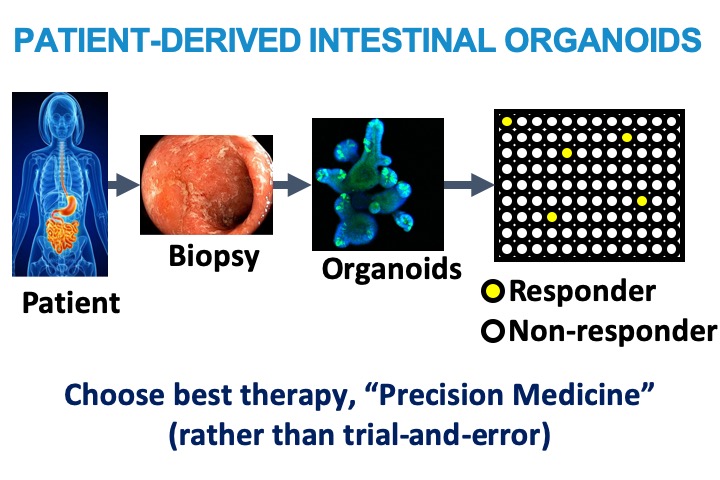
INTESTINAL ORGANOIDS
We are growing intestinal organoids from patients with and without IBD. Intestinal organoids are 3-dimensional cultures of primary intestinal epithelial cells (IECs) that we can grow in the lab. These organoids, derived directly from patients, provide a truly unique opportunity for precision medicine. We are developing a type of "living biobank" and testing how cells from different patients respond to a variety of inflammatory stimuli.
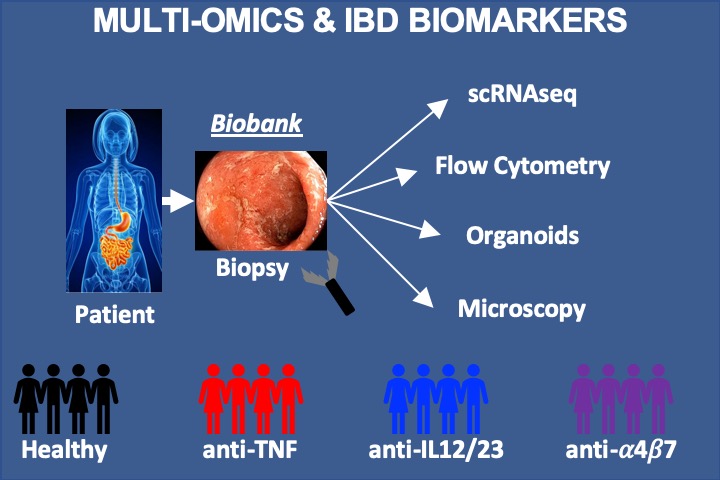
MULTI-OMICS APPROACHES FOR IBD
Gastroenterologists currently use a “trial-and-error” approach in treating IBD. In contrast, precision medicine would identify the best treatment for each patient up front. Using powerful new "multi-omics" approaches, we are studying the genes and cells in the blood and intestine of patients with and without IBD. These large datasets will help identify biomarkers that predict response to specific medications.
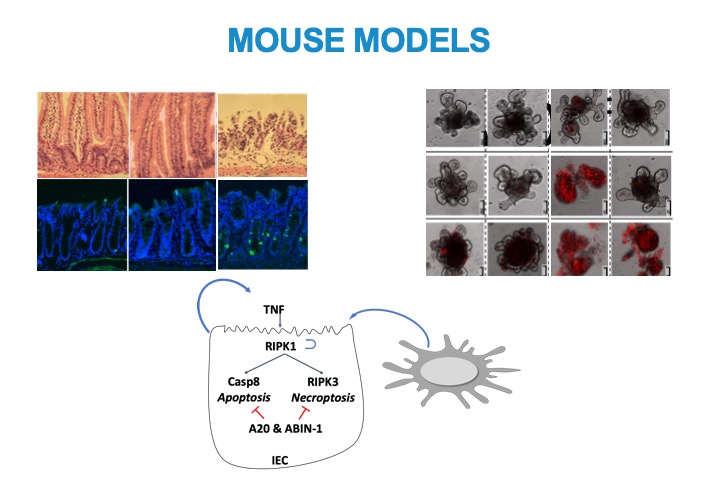
MOUSE MODELS
We have developed a mouse model that provides a unique opportunity to study both TNF-dependent and TNF-independent IEC death.